Abstract
Background
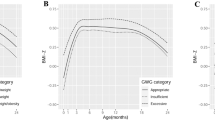
The aims of the study were to: (a) describe BMI-for-age trajectories in children up to four years of age; (b) evaluate the association between prepregnancy maternal BMI and the BMI-for-age trajectories.
Methods
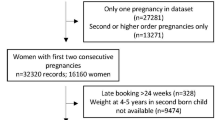
Data from 3218 (75.3% of the original cohort) children from the Pelotas 2015 Birth Cohort were analyzed. Prepregnancy BMI (kg/m2) was measured on the perinatal interview. Z-scores of BMI-for-age were calculated for children at three months, 1, 2 and 4 years. Trajectories were identified using a semi-parametric group-based modeling approach. Multinomial logistic regression was used to test the association between prepregnancy BMI (weight excess: BMI ≥ 25 kg/m2) and BMI-for-age trajectories.
Results
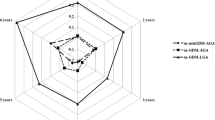
Four trajectories of the BMI-for-age, in z-score, were identified and represent children in the “increasing”, “adequate”, “stabilized” and “risk for weight excess” group. A total of 196 children (7.1%) belonged to the group that was at risk of weight excess. Adjusted analyses showed that children whose mothers presented prepregnancy weight excess had 2.36 (95%CI 1.71; 3.24) times more risk of belonging to group “risk for weight excess” when compared to those children whose mothers presented underweight/normal weight before pregnancy.
Conclusion
The risk of weight excess in children up to 4 years of age were greater in mothers who presented prepregnancy weight excess.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
The data underlying this article were provided by “Pelotas Birth Cohort, 2015” conducted by Postgraduate Program in Epidemiology at Universidade Federal de Pelotas. Information on how to access the data can be found at: https://www.epidemio-ufpel.org.br/site/content/home/.
References
Vézina-Im L-A, Nicklas TA, Baranowski T. Intergenerational effects of health issues among women of childbearing age: a review of the recent literature. Curr Nutr Rep. 2018;7:274–85. https://link.springer.com/10.1007/s13668-018-0246-x.
The GBD 2015 Obesity Collaborators. Health effects of overweight and obesity in 195 countries over 25 years. N Engl J Med. 2017;377:13–27. https://doi.org/10.1056/NEJMoa1614362.
Hinkle SN, Sharma AJ, Kim SY, Park S, Dalenius K, Brindley PL, et al. Prepregnancy obesity trends among low-income women, United States, 1999–2008. Matern Child Health J. 2012;16:1339–48. http://link.springer.com/10.1007/s10995-011-0898-2.
Black RE, Victora CG, Walker SP, Bhutta ZA, Christian P, de Onis M, et al. Maternal and child undernutrition and overweight in low-income and middle-income countries. The Lancet. 2013;382:427–51. Available from: https://linkinghub.elsevier.com/retrieve/pii/S014067361360937X.
Heerman WJ, Bian A, Shintani A, Barkin SL. Interaction between maternal prepregnancy body mass index and gestational weight gain shapes infant growth. Acad Pediatr. 2014;14:463–70. Available from: https://linkinghub.elsevier.com/retrieve/pii/S1876285914001429.
Leonard SA, Rasmussen KM, King JC, Abrams B Trajectories of maternal weight from before pregnancy through postpartum and associations with childhood obesity. Am J Clin Nutr. 2017;ajcn158683. Available from: https://doi.org/10.3945/ajcn.117.158683.
Chaparro MP, Koupil I, Byberg L. Maternal pre-pregnancy BMI and offspring body composition in young adulthood: the modifying role of offspring sex and birth order. Public Health Nutr. 2017;20:3084–9. https://www.cambridge.org/core/product/identifier/S1368980017002191/type/journal_article.
Castillo H, Santos IS, Matijasevich A. Relationship between maternal pre‐pregnancy body mass index, gestational weight gain and childhood fatness at 6–7 years by air displacement plethysmography. Matern Child Nutr. 2015;11:606–17. https://doi.org/10.1111/mcn.12186.
Cadenas-Sanchez C, Henriksson P, Henriksson H, Nyström CD, Pomeroy J, Ruiz JR, et al. Eur J Clin Nutr. 2017;71:1200–5. https://www.nature.com/articles/ejcn201762.
Albuquerque D, Nóbrega C, Manco L, Padez C. The contribution of genetics and environment to obesity. Br Med Bull. 2017;123:159–73. https://academic.oup.com/bmb/article/123/1/159/3930933.
Silventoinen K, Rokholm B, Kaprio J, Sørensen TIA. The genetic and environmental influences on childhood obesity: a systematic review of twin and adoption studies. Int J Obes. 2010;34:29–40.
Mameli C, Mazzantini S, Zuccotti G. Nutrition in the first 1000 days: the origin of childhood obesity. IJERPH. 2016;13:838. http://www.mdpi.com/1660-4601/13/9/838.
Dalrymple KV, Flynn AC, Seed PT, Briley AL, O’Keeffe M, Godfrey KM et al. Associations between dietary patterns, eating behaviours, and body composition and adiposity in 3‐year‐old children of mothers with obesity. Pediatr Obesity. 2020;15. Available from: https://doi.org/10.1111/ijpo.12608.
Voerman E, Santos S, Patro Golab B, Amiano P, Ballester F, Barros H et al. Maternal body mass index, gestational weight gain, and the risk of overweight and obesity across childhood: An individual participant data meta-analysis. Ma RCW, editor. PLoS Med. 2019;16:e1002744. Available from: https://dx.plos.org/10.1371/journal.pmed.1002744.
Bertoldi AD, Barros FC, Hallal PRC, Mielke GI, Oliveira PD, Maia MFS. et al. Trends and inequalities in maternal and child health in a Brazilian city: methodology and sociodemographic description of four population-based birth cohort studies, 1982–2015. Int J Epidemiol. 2019;48(Supplement_1):i4–i15. https://academic.oup.com/ije/article/48/Supplement_1/i4/5382480.
Hallal PC, Bertoldi AD, Domingues MR, Silveira MF, Demarco FF, da Silveira MF, et al. Cohort profile: the 2015 Pelotas (Brazil) birth cohort study. Int J Epidemiol. 2018;47:1048. https://academic.oup.com/ije/article/47/4/1048/4591650.
https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight Obesity and overweight.
World Health Organization (WHO). Anthro for personal computers, version 2, 2007: Software for assessing growth and development of the world’s children. Geneva: WHO; 2007. Avaliable in: http://www.who.int/childgrowth/software/en/.
World Health Organization (WHO). Multicentre Growth Reference Study Group. WHO child growth standards based on length/height, weight, and age. Acta Paediatr 2006; 76-85.
Nagin DS Group-Based Modeling of Development. Cambridge, MA: Harvard University Press. 2005.
Nagin DS, Odgers CL. Group-based trajectory modeling in clinical research. Annu Rev Clin Psychol. 2010;6:109–38.
Nagin D, Tremblay RE. Trajectories of boys’ physical aggression, opposition, and hyperactivity on the path to physically violent and nonviolent juvenile delinquency. Child Dev. 1999;70:1181–96.
Baker JL, Michaelsen KF, Rasmussen KM, Sørensen TIA. Maternal prepregnant body mass index, duration of breastfeeding, and timing of complementary food introduction are associated with infant weight gain. Am J Clin Nutr. 2004;80:1579–88.
Taveras EM. Childhood obesity risk and prevention: shining a lens on the first 1000 days. Child Obes. 2016;12:159–61. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4876524/.
Blake-Lamb TL, Locks LM, Perkins ME, Woo Baidal JA, Cheng ER, Taveras EM. Interventions for childhood obesity in the first 1,000 days a systematic review. Am J Prev Med. 2016;50:780–9.
Woo Baidal JA, Locks LM, Cheng ER, Blake-Lamb TL, Perkins ME, Taveras EM. Risk factors for childhood obesity in the first 1,000 days: a systematic review. Am J Prev Med. 2016;50:761–79.
Diet, nutrition and the prevention of chronic diseases: report of a joint WHO/FAO expert consultation, Geneva, 28 January - 1 February 2002 [Internet]. [cited 2022 Aug 22]. Available from: https://www.who.int/publications-detail-redirect/924120916X.
Ogden CL, Carroll MD, Kit BK, Flegal KM. Prevalence of childhood and adult obesity in the United States, 2011–2012. JAMA. 2014;311:806. https://doi.org/10.1001/jama.2014.732.
Yang Z, Huffman SL. Nutrition in pregnancy and early childhood and associations with obesity in developing countries: early nutrition and obesity. Matern Child Nutr. 2013;9:105–19. https://doi.org/10.1111/mcn.12010.
Brown WJ, Flores TR, Keating SE, Mielke GI. Trajectories and determinants of weight gain in two cohorts of young adult women born 16 years apart. Int J Obes. 2021;45:1553–64.
Connor Gorber S, Tremblay M, Moher D, Gorber B. A comparison of direct vs. self-report measures for assessing height, weight and body mass index: a systematic review. Obes Rev. 2007;8:307–26.
Carrilho TRB, Rasmussen KM, Farias DR, Costa NCF, Batalha MA, Reichenheim ME, et al. Agreement between self-reported pre-pregnancy weight and measured first-trimester weight in Brazilian women. BMC Pregnancy Childbirth. 2020;20:734.
Perumal N, Roth DE, Perdrizet J, Barros AJD, Santos IS, Matijasevich A, et al. Effect of correcting for gestational age at birth on population prevalence of early childhood undernutrition. Emerg Themes Epidemiol. 2018;15:3.
Acknowledgements
This article is based on data from the study “Pelotas Birth Cohort, 2015” conducted by Postgraduate Program in Epidemiology at Universidade Federal de Pelotas, with the collaboration of the Brazilian Public Health Association (ABRASCO). The first phases of the 2015 Pelotas (Brazil) Birth Cohort was funded by the Wellcome Trust (095582). Funding for specific follow-up visits was also received from the Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq) and Fundação de Amparo a Pesquisa do Estado do Rio Grande do Sul (FAPERGS) and Children’s Pastorate sponsored follow-up at twenty-four months; and FAPERGS – PPSUS, the Wellcome Trust (10735_Z_18_Z), and the Bernard van Leer Foundation (BRA-2018-178) for the fort-eight months follow-up.
Author information
Authors and Affiliations
Contributions
TRF, OAAL, MRD, MFS, PCH and ADB worked in the fieldwork and data collection of the 2015 Cohort. TRF and OAAL contributed to the conception and design of this study. TRF, OAAL, BPN and GIM conducted the statistical analyses and all authors contributed to the interpretation of findings. TRF conducted the research for related literature and wrote the initial draft of the paper. All authors contributed to subsequent versions, critically reviewed the paper several times, and approved the final version.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Flores, T.R., de Andrade Leão, O.A., Nunes, B.P. et al. Prepregnancy maternal BMI and trajectories of BMI-for-age in children up to four years of age: findings from the 2015 Pelotas (Brazil) birth cohort. Int J Obes 48, 353–359 (2024). https://doi.org/10.1038/s41366-023-01422-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-023-01422-1